Pandemic influenza awareness week. Day 1: History of pandemic influenza
It’s hard to avoid hearing about influenza virus these days. In all the noise, it’s tough to sort out the facts from the rumors and conspiracy theories. I’ve already discussed a bit about the basic biology of the virus in this post, so I'm not going to review that here (though a good overview can be found here for those of you who need to bone up on your influenza virus biology). So, this week, as a part of Pandemic influenza awareness week, I’ll be writing a 5-part series about various issues regarding influenza. Today, I’ll discuss the history of influenza, focusing on past pandemics. The rest of the week will address the following topics, with the goal of presenting a review of the facts without the scare-mongering:
"Avian flu" and H5N1, 1997-present
How do we prevent/control a pandemic? What models and surveillance can tell us
Where we are now—are we ready for a pandemic?
Other issues in influenza
So, without further ado, let's dive into today's topic:
A quick trip through the history of pandemic influenza
Influenza is an ancient disease. It is first described by Hippocrates in 412 BC, though the term "influenza" would not be coined until the 14th century. ("Influenza" is Italian for "influence," as the prevailing idea of disease causation at that time was the influence of the stars). In 1580, a disease originating from Asia and thought to be influenza swept through Europe, Africa, and the Americas on trade routes. While these cannot be confirmed as influenza, a better handle on the symptoms of the disease makes it likely that several influenza pandemics occurred in the 1800s: in 1833, 1836, 1847 and 1889.
The worst influenza pandemic in recorded history took place in 1918-1919. At least 40 million, and likely closer to 100 million deaths worldwide have been attributed to the virus, most of them occurring in the 16-week period between September-December 1918. In large U.S cities, more than 10,000 deaths per week were attributed to the virus. It is estimated that as many as 50% of the population was infected, and ~1% died. To compare, in “normal” (interpandemic) years, it is estimated that between 10-20% of the population is infected, with a .008% mortality.
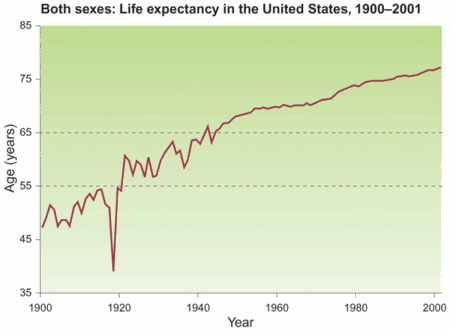
Despite its popular name of the “Spanish flu,” it’s uncertain where the pandemic originated. (During World War I, Spain was one of the few countries who did not censor media, so reports of the state of the epidemic in that country were widely circulated). Scientists and historians have put forth points of origin in China, Vietnam, India, France, Great Britain, and the U.S. (Kansas). Contemporary reports of the pandemic contain imagery that harkens back to the 14th century Black Plague. Morgues were overwhelmed; dead were buried in simple pine boxes, as the supply of caskets was quickly depleted; public activities were cancelled; spitting on the street was criminalized. The death toll made the casualties as a result of World War I pale by comparison. The virus struck hardest in the young and healthy, whose rapid immune response actually became their downfall. Enough young people died that it dramatically decreased the average life expectancy in that year (see figure below, from Nature Medicine 10, S82 - S87 (2004)).
Typically, influenza causes death due to a secondary bacterial pneumonia. Bacteria are able to take advantage of the host’s compromised immune status and damaged lung cells, establishing a potentially deadly infection. However, during the 1918 pandemic, a greater percentage of the deaths in the 20-45 age group were due to primary pneumonia: pneumonia caused by a combination of the influenza virus and the host response, with no bacterial invaders involved. In some patients, this occurred within a matter of hours from the first symptoms. A Pennsylvania medical student documented the phenomenon:
Though serological studies carried out in the 1930s had already identified the virus as a serotype H1N1, it was long thought that was the end of the potential information that could be found about the virus. However, in the mid-1990s, a group of researchers led by Jeffrey Taubenberger at the Armed Forces Institute of Pathology found samples of lung tissue from soldiers who had died of the 1918 virus in the archive at that institute. Additionally, pathologist Johan Hultin provided an additional sample from the lungs of an Inuit woman in Alaska who had died during the pandemic. These samples have been sequenced in an effort to determine what it was that made the 1918 virus so virulent. Though these questions are still being investigated, the preliminary data suggests that the virus was a human-avian reassortant which had entered the human population a short time before the pandemic (likely 6-12 months).
Though the 1918 pandemic has been the most dramatic example of the killing potential of influenza, there have been 2 other pandemics in the last 100 years. In 1957, a H2N2 virus appeared in China. This “Asian flu” quickly swept through the population, replacing the previously-circulating H1N1 virus and killing 70,000 in the U.S. Similarly, in 1968, an H3N2 virus emerged from Hong Kong to replace the H2N2 virus. This pandemic resulted in 34,000 American deaths. The H1N1 serotype re-surfaced in 1977, and currently, H3N2, H1N1, and reassortant H1N2 viruses circulate in the human population.
The H1N1 caused an additional scare in 1976. In January of that year, a private at Fort Dix, New Jersey, collapsed and died following a march. It was determined that he died of “swine flu,” serotype H1N1. Although he was the only death at the fort, health officials were highly concerned. Secretary of health F. David Matthews stated that
With hindsight, we can see that a proclamation with this level of certainty is folly, but at the time, it was thought that influenza cycled in a fairly regular pattern, varying between very high pathogenicity strains and lower pathogenicity strains. It was thought that the world was overdue for another high pathogenicity strain, and that the “swine flu” virus just might be the one. In March of 1976, President Ford announced that he would ask Congress for funds to produce enough vaccine “to inoculate every man, woman, and child in the United States.” Of course, this epidemic never materialized, and actually dealt a blow to the influenza vaccine campaign, as reported side effects of the vaccine included Guillain-Barré syndrome, a debilitating neurologic condition.
Looking back, one can certainly draw parallels between the scare and build-up to vaccination in 1976 and today with H5N1. However, just because that pandemic never materialized does not mean that the same thing will happen with today’s “avian flu.” At this point, we just don’t know, but it behooves us to hope for the best, but prepare for the worst.
Tomorrow: all about avian flu and H5N1, from its initial identification in 1997 to today.
More resources on pandemic influenza:
CIDRAP Pandemic influenza news
Infectious Disease Society of America (IDSA) Pandemic/Avian flu
CDC's site on Avian flu
Flu wiki
So, without further ado, let's dive into today's topic:
A quick trip through the history of pandemic influenza
Influenza is an ancient disease. It is first described by Hippocrates in 412 BC, though the term "influenza" would not be coined until the 14th century. ("Influenza" is Italian for "influence," as the prevailing idea of disease causation at that time was the influence of the stars). In 1580, a disease originating from Asia and thought to be influenza swept through Europe, Africa, and the Americas on trade routes. While these cannot be confirmed as influenza, a better handle on the symptoms of the disease makes it likely that several influenza pandemics occurred in the 1800s: in 1833, 1836, 1847 and 1889.
The worst influenza pandemic in recorded history took place in 1918-1919. At least 40 million, and likely closer to 100 million deaths worldwide have been attributed to the virus, most of them occurring in the 16-week period between September-December 1918. In large U.S cities, more than 10,000 deaths per week were attributed to the virus. It is estimated that as many as 50% of the population was infected, and ~1% died. To compare, in “normal” (interpandemic) years, it is estimated that between 10-20% of the population is infected, with a .008% mortality.
Despite its popular name of the “Spanish flu,” it’s uncertain where the pandemic originated. (During World War I, Spain was one of the few countries who did not censor media, so reports of the state of the epidemic in that country were widely circulated). Scientists and historians have put forth points of origin in China, Vietnam, India, France, Great Britain, and the U.S. (Kansas). Contemporary reports of the pandemic contain imagery that harkens back to the 14th century Black Plague. Morgues were overwhelmed; dead were buried in simple pine boxes, as the supply of caskets was quickly depleted; public activities were cancelled; spitting on the street was criminalized. The death toll made the casualties as a result of World War I pale by comparison. The virus struck hardest in the young and healthy, whose rapid immune response actually became their downfall. Enough young people died that it dramatically decreased the average life expectancy in that year (see figure below, from Nature Medicine 10, S82 - S87 (2004)).

Typically, influenza causes death due to a secondary bacterial pneumonia. Bacteria are able to take advantage of the host’s compromised immune status and damaged lung cells, establishing a potentially deadly infection. However, during the 1918 pandemic, a greater percentage of the deaths in the 20-45 age group were due to primary pneumonia: pneumonia caused by a combination of the influenza virus and the host response, with no bacterial invaders involved. In some patients, this occurred within a matter of hours from the first symptoms. A Pennsylvania medical student documented the phenomenon:
As their lungs filled, the patients became short of breath and increasingly cyanotic. After gasping for several hours, they became delirious and incontinent, and many died struggling to clear their airways of a blood-tinged froth that sometimes gushed from their nose and mouth. It was a dreadful business.
Though serological studies carried out in the 1930s had already identified the virus as a serotype H1N1, it was long thought that was the end of the potential information that could be found about the virus. However, in the mid-1990s, a group of researchers led by Jeffrey Taubenberger at the Armed Forces Institute of Pathology found samples of lung tissue from soldiers who had died of the 1918 virus in the archive at that institute. Additionally, pathologist Johan Hultin provided an additional sample from the lungs of an Inuit woman in Alaska who had died during the pandemic. These samples have been sequenced in an effort to determine what it was that made the 1918 virus so virulent. Though these questions are still being investigated, the preliminary data suggests that the virus was a human-avian reassortant which had entered the human population a short time before the pandemic (likely 6-12 months).
Though the 1918 pandemic has been the most dramatic example of the killing potential of influenza, there have been 2 other pandemics in the last 100 years. In 1957, a H2N2 virus appeared in China. This “Asian flu” quickly swept through the population, replacing the previously-circulating H1N1 virus and killing 70,000 in the U.S. Similarly, in 1968, an H3N2 virus emerged from Hong Kong to replace the H2N2 virus. This pandemic resulted in 34,000 American deaths. The H1N1 serotype re-surfaced in 1977, and currently, H3N2, H1N1, and reassortant H1N2 viruses circulate in the human population.
The H1N1 caused an additional scare in 1976. In January of that year, a private at Fort Dix, New Jersey, collapsed and died following a march. It was determined that he died of “swine flu,” serotype H1N1. Although he was the only death at the fort, health officials were highly concerned. Secretary of health F. David Matthews stated that
there is evidence there will be a major flu epidemic this coming fall. The indication is that we will see a return of the 1918 flu virus that is the most virulent form of flu. In 1918, half a million people died. The projections are that this virus will kill one million Americans in 1976.
With hindsight, we can see that a proclamation with this level of certainty is folly, but at the time, it was thought that influenza cycled in a fairly regular pattern, varying between very high pathogenicity strains and lower pathogenicity strains. It was thought that the world was overdue for another high pathogenicity strain, and that the “swine flu” virus just might be the one. In March of 1976, President Ford announced that he would ask Congress for funds to produce enough vaccine “to inoculate every man, woman, and child in the United States.” Of course, this epidemic never materialized, and actually dealt a blow to the influenza vaccine campaign, as reported side effects of the vaccine included Guillain-Barré syndrome, a debilitating neurologic condition.
Looking back, one can certainly draw parallels between the scare and build-up to vaccination in 1976 and today with H5N1. However, just because that pandemic never materialized does not mean that the same thing will happen with today’s “avian flu.” At this point, we just don’t know, but it behooves us to hope for the best, but prepare for the worst.
Tomorrow: all about avian flu and H5N1, from its initial identification in 1997 to today.
More resources on pandemic influenza:


